Trochanteric Pain Syndrome (TPS) colloquially known as “Trochanteric Bursitis” refers to conditions that lead to pain over the greater trochanter of the upper femur (thigh bone) – this is the bony prominence on the outside of the hip. Most commonly this involves inflammation of one of the bursae (bursitis) of the hip but other tissues in the area can be affected. The bone of the trochanter itself can be a source of pain (fractures, local bone lesions), the gluteal tendons which insert into the trochanter (tendinopathy, tendon tears, calcific tendinopathy) and the fascial tissue of the outside of the thigh – the fascia lata/iliotibial band complex – (fascial tightness, “snapping” hip). TPS can result from a problem with one of these tissues or can be due to multiple local tissue pathologies acting in concert.
A bursa is a filmy sac of tissue that contains a tiny amount of fluid. It acts as a cushion that protects the bone from excessive pressure from overlying moving soft tissues. Bursa are present in the body wherever there are bony prominences close to joints – over the front of the knee (pre-patellar bursa), over the point of the elbow (olecranon bursa) and over the side of the shoulder (subdeltoid bursa). On the outside of the hip, there are 2 bursae – the superficial trochanteric bursa which protects the bone from the fascia lata/iliotibial band and the deeper subgluteal bursa which lies between the gluteal tendons and the bone. The term “trochanteric bursitis” refers to inflammation of one or both of these 2 lateral hip bursae.
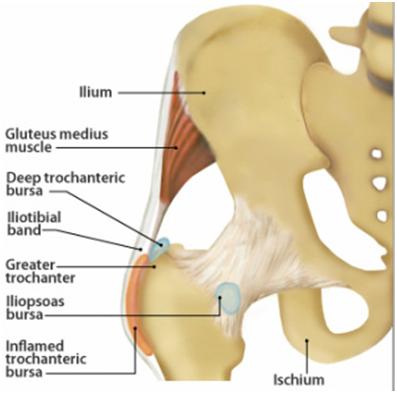
Figure 1. The Anatomy of the Trochanteric Region inc. the bony greater trochanter, soft tissues and bursae.
The cause of trochanteric bursitis is idiopathic in most cases – this means there is no identifiable reason. Idiopathic trochanteric bursitis occurs most commonly in females (? Increased pelvic width compared with males), in older age groups (50 -75 years – associated with degenerative soft tissue changes) and there is unquestionably an association with obesity (increased soft tissue load with weight bearing activity). Tightness of the fascia lata/iliotibial band complex can be identified in many patients with this condition. Trochanteric bursitis can occur after trauma to the outside of the hip (a fall or direct blow) or after lying on the side of the hip for a prolonged period. Inflammatory conditions such as rheumatoid arthritis can cause local bursal inflammation. Bone spurs on the trochanter and calcium deposits in the bursa itself can lead to bursitis. Bursitis can follow hip surgery, particularly hip replacement and hip fracture fixation.
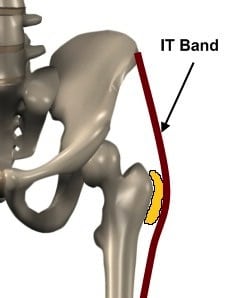
Figure 2. The relationship of the iliotibial band and the superficial trochanteric bursa.
Gluteal tendon abnormalities can cause trochanteric pain, but rarely in isolation. The gluteus medius tendon attaches to the superficial surface of the greater trochanter whereas the gluteus minimus tendon attaches to the deep surface. The gluteus maximus tendon inserts into the upper part of the femur and is not usually implicated in TPS. Tendon tears can be a result of an acute injury (generally younger athletic individuals) but much more commonly are part of a degenerative process that occurs with ageing. Internal degeneration of intact tendons (tendinopathy) can be present and degenerative tendon tears are very common in individuals above the age of fifty – only a small proportion of these are actually painful – probably a result of an associated bursitis or impingement (abnormal contact or pinching) against the overlying fascial tissue.
Snapping hip is generally a condition that affects young and generally athletic/active females. It is caused by the fascia lata/iliotibial band, which is a large sheet of fibrous tissue on the outside of the leg, snapping or audibly rubbing against the greater trochanter with repeated flexion and extension of the hip. This snapping may or may not be painful. The bursa can be caught in between and become inflamed as part of a “friction” type syndrome.
Trochanteric Pain Syndrome is characterised by pain over the lateral aspect or “point” of the hip. It can radiate sometimes along the outer aspect of the thigh or into the buttock. It is usually dull and aching but the outside of the hip can be quite tender to touch. Generally this causes most trouble at night when lying on the affected side – which is either not possible at all or only for a very short time. Some individuals find they are unable to lie on the opposite side for any period – this position will also cause pain to arise in the affected hip. This nocturnal pain can cause major disruption to sleep and is often the main driving reason for seeking treatment. Pain can be present with sitting, particularly when driving for significant distances. When bad, pain can be present even with walking, stair climbing or any activities involving repetitive hip flexion and extension.
Examination of an individual with suspected TPS should include an observation of gait, palpation over affected site for the extent of tenderness, assessment of the range of motion of the hip (noting painful positions) and the strength of the various muscle groups supporting the hip, particularly the gluteal muscles. A test for fascial tightness is very helpful and this maneouvre will often reproduce pain typical of TPS. Snapping of the fascia over the greater trochanter can often be demonstrated by the individual, if present.
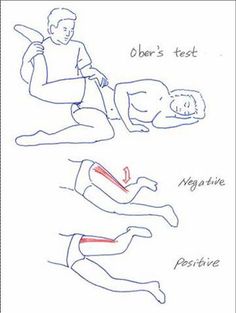
Figure 3. Ober’s Test for fascial/ilotibial band tightness.
Radiological investigations are very helpful in determining the tissues involved and their pathologies in each case of TPS. Plain xrays are important for ruling out hip joint disease but also show any irregularities on the external surface of the greater trochanter, together with calcific deposits in the adjacent soft tissues and any local bone lesions within the trochanter itself. Ultrasound is a popular investigation but does have significant limitations. It may reveal fluid in the trochanteric bursa and can demonstrate tendon pathology, but its diagnostic accuracy is variable. MRI is the investigation of choice as it can show all forms of pathology in both the soft and bony tissues of the trochanteric region as well as the hip joint itself.
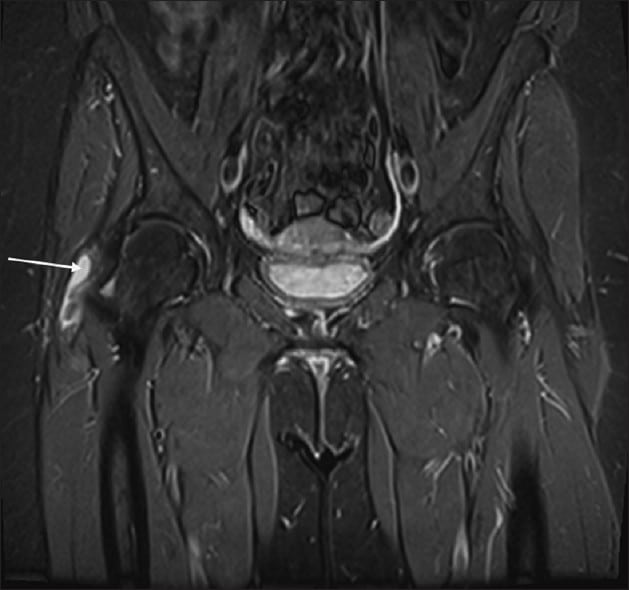
Figure 4. MRI scan indicating fluid in an inflamed trochanteric bursa (left) and no fluid (right).
The natural history of TPS, even if untreated, is usually one of slow resolution over a period of months to years. The treatment of TPS may change slightly depending on the diagnosis as to the cause/pathology present, but in general follows some basic principles. In almost every case, conservative or non-operative treatment is the appropriate first line management. It may seem obvious, but avoidance of situations that cause pain is essential – continuing with painful activity will never allow this condition to settle. This usually means adopting a comfortable sleeping position at night – avoiding lying on the affected side, putting a pillow between the legs if lying on the opposite side or lying on the back to avoid direct pressure on the painful area. Correction of associated underlying conditions – weight loss in obese individuals and rheumatological review/treatment of established generalized inflammatory disorders when present (eg. rheumatoid arthritis) is very important. Local physical treatment in the form of stretches to the fascia lata/ilio-tibial band complex and gentle eccentric gluteal and core strengthening can be very helpful, particularly when able to be undertaken comfortably. Instruction from a therapist regarding the use of a foam roller or similar device over the trochanter and fascia can complement an exercise program.
Figure 5. Stretches to the fascia/iliotibial band complex using a foam roller.
Analgesic medication and local heat can reduce the pain of TPS. Non-steroidal anti-inflammatory drugs (NSAIDs) can be useful in inflammatory tendon/bursal conditions. Cortisone injections into the trochanteric and subgluteal bursae (under ultrasound control to ensure accuracy of delivery) are often more effective than NSAIDs and don’t generally have the same potential for side effects. Reducing pain in this way to enable satisfactory participation in a stretching/strengthening exercise program can be one of the keys to successful treatment. Sometimes multiple cortisone injections are required, spread out over a period of time. Injections of autologous blood (patients own blood) or platelet rich plasma may be indicated in TPS where tendinopathy/tendon tears seem to be the predominant pathology.
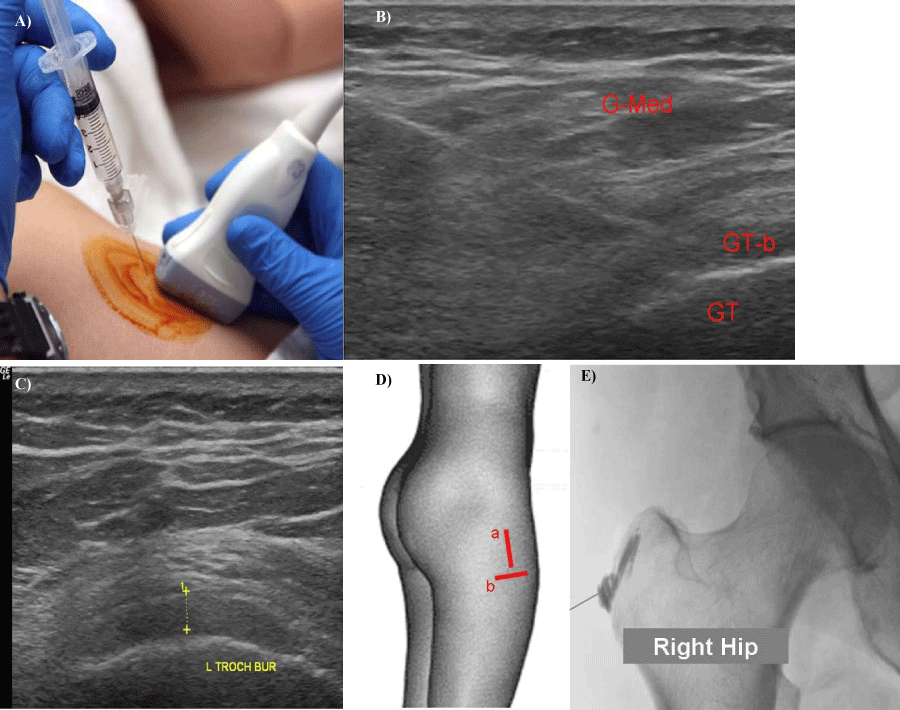
Figure 6. Ultrasound guided injection of local anaesthetic and steroid into the trochanteric bursa.
Surgical treatment of TPS is rarely required or indicated. Surgery unfortunately is not always successful and it is impossible to predict the outcome pre-operatively. Recovery is generally slow and often involves a period of non-weight bearing on crutches followed by an extensive rehab/physiotherapy program together with a lot of patience. Despite undertaking all the correct steps, a proportion of individuals with TPS undergoing surgery will still continue to have pain and functional limitation. If surgery is to be undertaken, identification of all the pathologies involved and addressing each of these with the operative procedure is important. Surgery clearly carries some risk – infection, deep vein thrombosis, nerve or vessel damage and anaesthetic complications are possible – and is always absolutely a last resort attempt at symptom improvement in most cases of TPS.
Source: https://www.parkclinic.com.au/trochanteric-pain-syndrome/